-
Shop by category
- Accessories (23)
- Anti-Aging Products (432)
- Anti-Wrinkle Treatment Products (149)
- Biorevitalization (6)
- Botulinum Toxin (12)
- Chemical Peels (44)
- Dermal Fillers (76)
- Fat Dissolving / Lipolysis (10)
- Fillers For Body (5)
- Skin Boosters (34)
- Skin Moisturizers (115)
- Under Eye Creams (33)
- Excessive Facial Hair Inhibitors (5)
- Eye Care (26)
- Eyelash Growth Products (7)
- Hair Care, Treatment & Hair Growth Products (59)
- Men’s Health Products (25)
- Oral Care Products (22)
- Pet Health (2)
- Skin Care Products (284)
- Skin Lightening Products (209)
- Slider (0)
- Supplements & Drugs (374)
- Allergy (12)
- Anti-Addiction (5)
- Anti-Influenza (1)
- Antibiotics (46)
- Asthma (34)
- Brain & Antidepressants (33)
- Cancer Treatment (28)
- Diabetes (11)
- Heart / Blood Pressure (15)
- HIV, AIDS, Herpes & Hepatitis Treatment Medications (22)
- Homoeopathy (64)
- Immunosuppressants (11)
- Migraine (6)
- Thyroid Extract Supplements (7)
- Vitamins & Minerals (87)
- Wilson’s Disease (3)
- Topical Anesthetics / Pain Management (37)
- Weight Loss Treatment Products (22)
- Women's Health Products (62)
- Contraceptives / Birth Control Pills (21)
- Endocrine System (21)
- Sexual Wellness (13)
✓ We Dispatch The Freshest Batch
✓ Discreet Shipping Within 24h Daily
✓ Great Customer Service
✓ Competitive prices on all products
Diabetes
Showing all 11 results
-
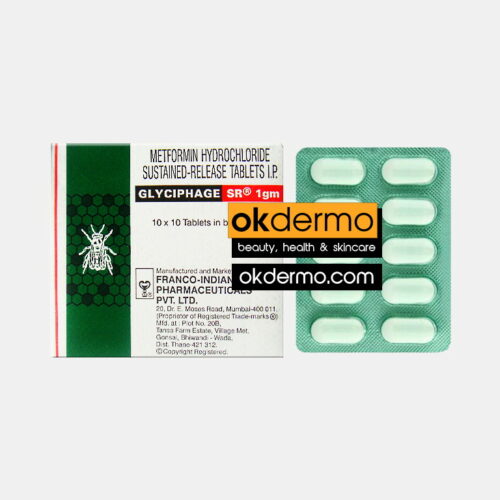
Metformin Tablets
Metformin HCl 250mg / 500mg / 1g
Size: 60 tablets
Brand name: Glucophage, Glumetza, Riomet
From USD $15.00 Select options -
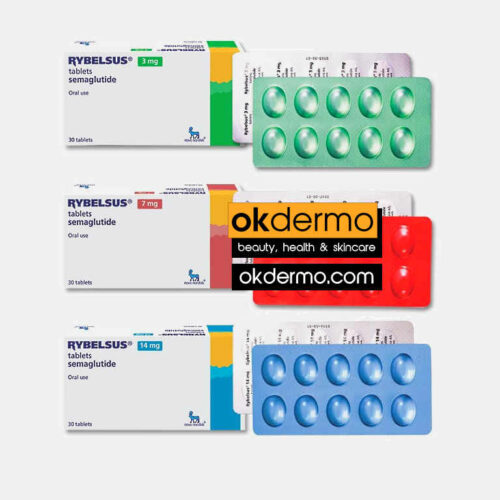
Rybelsus® Semaglutide Tablets
Semaglutide 3mg / 7mg / 14mg
Size: 30 Tablets
Brand name: Rybelsus, Ozempic, Wegovy
From USD $345.00 Select options -
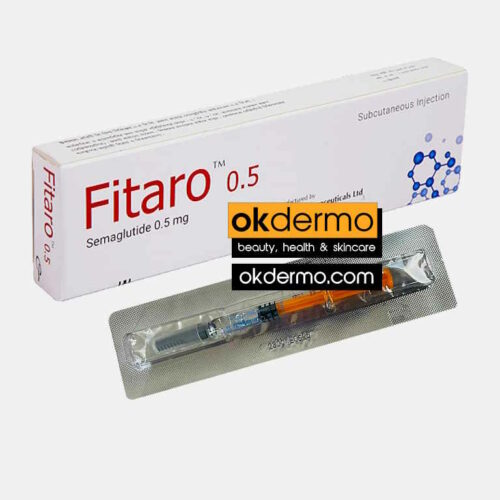
Fitaro® Semaglutide Subcutaneous Injection
Semaglutide 0.25mg / 0.50mg / 1mg / 1.7mg / 2.4mg
Size: 1 Pre-Filled Injection Syringe
Brand name: Ozempic, Wegovy
From USD $141.00 Select options -
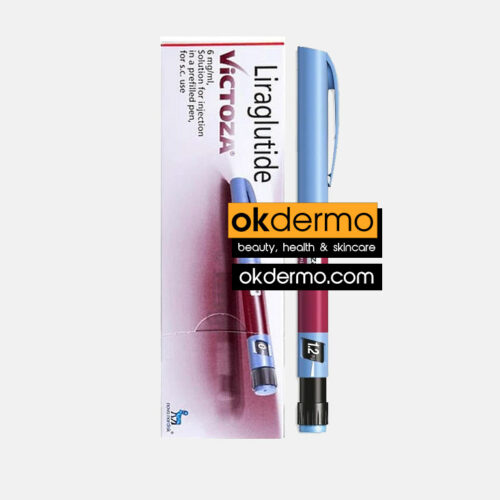
Victoza® Liraglutide Pre-Filled Pen
Liraglutide 6mg/ml Solution for Injection
Size: 3ml in 1 Pre-Filled Pen
Brand name: Saxenda
USD $231.00 Add to cart -

Saxenda® Liraglutide injection
Liraglutide 3mg
Size: 3ml/0.10fl.oz in 1 Pre-Filled Pen
Brand name: Victoza
USD $190.00 Add to cart -
Brom® Bromocriptine Tablets
Bromocriptine 2.5mg
Size: 30 Tablets
Brand name: Cycloset, Parlodel
USD $29.00 Add to cart -

Lobg® Lobeglitazone Tablets
Lobeglitazone Sulfate 0.5mg
Size: 30 Tablets
Brand name: Duvie
USD $27.00 Add to cart -
Jardiance® Empagliflozin Tablets
Empagliflozin 5mg / 10mg / 12.5mg / 25mg + Metformin 500mg / 1000mg
Size: 30 Tablets
Brand name: Jardiance
From USD $166.00 Select options -
Januvia® Sitagliptin Tablets
Sitagliptin 25mg / 50mg / 100mg + Dapagliflozin 5mg / 10mg
Size: 30 Tablets
Brand name: Januvia, Zituvio, Istavel, Auro-Sitagliptin, JAMP Sitagliptin, Taro-Sitagliptin Fumarate
From USD $44.00 Select options -
Pioglit® Pioglitazone Tablets
Pioglitazone 7.5mg / 15mg / 30mg
Size: 30 Tablets
Brand name: Actos
From USD $29.00 Select options -
Xultophy® Pre-Filled Pen Injection
Liraglutide 3.6mg/1ml + Insulin Degludec 100IU
Size: 3ml in 1 Pre-Filled Pen
USD $203.50 Add to cart

Diabetes is a disease that occurs when your blood glucose, also called blood sugar, is too high. Over time, having too much glucose in your blood can cause health problems.
About 10 percent of the people in the United States have diabetes, but about one in four people who have diabetes don’t know it.
Although diabetes has no cure, people with diabetes can take steps to manage their condition and stay healthy. Taking insulin or other diabetes medicines is often part of treating diabetes, along with healthy food choices and physical activity.
The most common type of diabetes is type 2 diabetes, in which your body does not make or use insulin well. This type of diabetes occurs most often in middle-aged and older people, but it can develop at any age, even in childhood.
You are more likely to develop type 2 diabetes if you are 45 years old or older, have a family history of diabetes, or are overweight. Physical inactivity, race, and certain health problems such as high blood pressure, prediabetes, or having had gestational diabetes while pregnant also affect your likelihood of developing type 2 diabetes.
For more information about diabetes and related conditions, see the National Institute of Diabetes and Digestive and Kidney Diseases Web site.
Nutrition and Physical Activity for People With Diabetes
Nutrition and physical activity are important parts of a healthy lifestyle for people with diabetes. Eating well and being physically active can help you.
- Keep your blood glucose level, blood pressure, and cholesterol in your target range.
- Lose weight or stay at a healthy weight
- Prevent or delay diabetes problems
- Feel good and have more energy
Type 2 Diabetes
Type 2 diabetes used to be called adult-onset diabetes but is becoming more common in children. This form of diabetes is caused when your body either resists insulin or doesn’t produce enough. It causes your blood glucose levels to be unbalanced.
There is no cure. However, many people are able to manage their blood glucose levels with diet, main supplements, and exercise. If not, a doctor can prescribe medications that can manage blood sugar levels. Some of these medications are:
- insulin therapy
- metformin (brand names: Glucophage, Glumetza, others)
- sulfonylureas
- meglitinides
A healthy diet, physical activity, and maintaining a healthy weight are the first, and sometimes, the most important part of diabetes treatment. However, when those are not enough to maintain your blood sugar levels, your doctor can decide which medications will work best for you.
Along with these treatments, people with diabetes have tried numerous herbs and supplements to improve their diabetes. These alternative treatments are supposed to help control blood sugar levels, reduce resistance to insulin, and prevent diabetes-related complications. Some supplements have shown promise in studies.
Using Supplements for Diabetes Treatment
It is always best to let the foods you eat provide your vitamins and minerals. However, more and more people are turning to alternative medicines and supplements. Supplements should not be used to replace standard diabetes treatment. Doing so can put your health at risk.
It is important to talk to your doctor before using any supplements. Some of these products can interfere with other treatments and medications. Just because a product is natural does not mean it is safe to use.
A number of supplements have shown promise as diabetes treatments. These include the following.
Cinnamon – Chinese medicine has been using cinnamon for medicinal purposes for hundreds of years. It has been the subject of numerous studies to determine its effect on blood glucose levels. A 2011 study has shown that cinnamon, in whole form or extract, helps lower fasting blood glucose levels. More studies are being done, but cinnamon is showing promise for helping to treat diabetes.
Chromium – is an essential trace element. It is used in the metabolism of carbohydrates. However, research on the use of chromium for diabetes treatment is mixed. Low doses are safe for most people, but there is a risk that chromium could make blood sugar go too low. High doses also have the potential to cause kidney damage.
Vitamin B-1 – is also known as thiamine. Many people with diabetes are thiamine deficient. This may contribute to some diabetes complications. Low thiamine has been linked to heart disease and blood vessel damage.
Thiamine is water-soluble. It has difficulty getting into the cells where it’s needed. However, benfotiamine, a supplemental form of thiamine, is lipid-soluble. It more easily penetrates cell membranes. Some research suggests that benfotiamine can prevent diabetic complications.
Alpha-Lipoic Acid (ALA) – is a potent antioxidant. Some studies suggest it may reduce oxidative stress, lower fasting blood sugar levels, and decrease insulin resistance. However, more research is needed. Furthermore, ALA needs to be taken with caution, as it has the potential to lower blood sugar levels to dangerous levels.
Bitter Melon – is used to treat diabetes-related conditions in countries like Asia, South America, and others. There is a lot of data on its effectiveness as a treatment for diabetes in animal and lab studies. However, there is limited human data on bitter melon.
Green Tea – contains polyphenols, which are antioxidants. The main antioxidant in green tea is known as epigallocatechin gallate (EGCG). Laboratory studies have suggested that EGCG may have numerous health benefits including lower cardiovascular disease risk, prevention of type 2 diabetes, improved glucose control, and better insulin activity.
Resveratrol – is a chemical found in wine and grapes. In animal models, it helps prevent high blood sugar. Animal studies have also shown that it can reduce oxidative stress. However, human data is limited.
Magnesium – is an essential nutrient. It helps regulate blood pressure. It also regulates insulin sensitivity. Supplemental magnesium may improve insulin sensitivity in diabetics.
A high magnesium diet may also reduce the risk of diabetes. Researchers have found a link between higher magnesium intake, lower rates of insulin resistance, and diabetes.
Probiotics – animal studies suggest that probiotics may decrease blood sugar by reducing inflammation and preventing the destruction of pancreatic cells that make insulin. Several other mechanisms may be involved as well.
American ginseng, a variety grown primarily in North America, has been shown to decrease post-meal blood sugar by about 20% in healthy individuals and those with type 2 diabetes.
Additionally, when people with type 2 diabetes took 1 gram of American ginseng 40 minutes before breakfast, lunch, and dinner for two months while maintaining their regular treatment, their fasting blood sugar decreased by 10% compared to those on a placebo. American ginseng may improve your cells’ response to and increase your body’s secretion of insulin
Aloe vera may also help those trying to lower their blood sugar. Supplements or juice made from the leaves of this cactus-like plant could help lower fasting blood sugar and A1C in people with prediabetes or type 2 diabetes. Mouse studies indicate that aloe may stimulate insulin production in pancreatic cells, but this hasn’t been confirmed.
In a review of nine studies in people with type 2 diabetes, supplementing with aloe for 4–14 weeks decreased fasting blood sugar by 46.6 mg/dl and A1C by 1.05%. People who had fasting blood sugar above 200 mg/dl before taking aloe experienced even stronger benefits.
Berberine isn’t a specific herb, but rather a bitter-tasting compound taken from the roots and stems of certain plants, including goldenseal and Phellodendron. Berberine may improve insulin sensitivity and enhance sugar uptake from your blood into your muscles, which helps lower blood sugar
A review of 27 studies in people with type 2 diabetes observed that taking berberine in combination with diet and lifestyle changes reduced fasting blood sugar by 15.5 mg/dl and A1C by 0.71% compared to diet and lifestyle changes alone or with a placebo. The review also noted that berberine supplements taken alongside diabetes medication helped lower blood sugar more than medication alone.
Vitamin D deficiency is considered a potential risk factor for type 2 diabetes. In one study, 72% of participants with type 2 diabetes were deficient in vitamin D at the start of the study. Vitamin D may improve the function of pancreatic cells that make insulin and increase your body’s responsiveness to insulin.
After two months of taking a 4,500-IU supplement of vitamin D daily, both fasting blood sugar and A1C improved. In fact, 48% of participants had an A1C that showed good blood sugar control, compared to only 32% before the study.
Gymnema Sylvestre – is an herb used as a diabetes treatment in the Ayurvedic tradition of India. The Hindu name for the plant – gurmar – means “sugar destroyer”. Gymnema Sylvestre may reduce sugar absorption in your gut and promote cells’ uptake of sugar from your blood. Due to its impact on type 1 diabetes, it’s suspected that Gymnema Sylvestre may somehow aid insulin-producing cells in your pancreas.
In one study, people with type 2 diabetes taking 400 mg of Gymnema leaf extract daily for 18–20 months experienced a 29% decrease in fasting blood sugar. A1C decreased from 11.9% at the start of the study to 8.48%. Further research suggests that this herb may help lower fasting blood sugar and A1C in type 1 (insulin-dependent) diabetes and may reduce cravings for sweets by suppressing the sweet-taste sensation in your mouth.
As you can see from this list, there are a number of natural supplements that can be used to manage diabetes. However, even for those on this list, it is important that you talk to your doctor before adding any supplement or vitamin to the diabetes plan.
There are a number of popular supplements that can have negative interactions with diabetes medications and blood sugar. Zinc is one of these popular supplements that can affect your blood glucose levels negatively. Even those on this list that can help many with diabetes may still have a negative interaction with some of your medications.















