Description
WHAT IS MELALONG MEQUINOL 2% + TRETINOIN 0.01% CREAM (Solage)
Combination of powerful components Mequinol and Tretinoin are used to treat areas of the skin that have become darker after repeated exposure to the sun. These areas are called solar lentigines, or age or liver spots. Mequinol is an active ingredient in Melalong cream used for skin depigmentation and it is mixed with tretinoin, a topical retinoid. A common formulation for this drug is an ethanolic solution of 2% mequinol and 0.01% tretinoin by mass. Dermatologists commonly prescribe the drug to treat solar lentigines, liver spots, or age spots.
Melalong cream is a 2-way combination cream made by Ajana company as an alternative/generic to famous Solage Cream. A cream containing the active ingredients Mequinol 2% (two percent) strength, a skin bleaching agent and tretinoin 0.01 percent strength, an artificially made form of vitamin A used to treat sun-damaged skin, also as peels and exfoliator, skin regenerator. Melalong medicated cream is a skin lightening agent and can be used in the gradual bleaching of hyperpigmented skin due to freckles and senile lentigines. Melalong cream can be used by people wishing for fairer skin and also for the treatment of chloasma and melasma conditions that causes dark patches on the face, especially the cheeks.
Lower dosages of mequinol have been used in conjunction with a Q-switched laser to depigment skin in patients with disseminated idiopathic vitiligo. Melalong (mequinol 2%, tretinoin 0.01%) Topical cream is indicated for the treatment of solar lentigines. Melalong should only be used under medical supervision as an adjunct to comprehensive skincare and sun avoidance program where the patient should primarily either avoid the sun or use protective clothing. Neither the safety nor effectiveness of Melalong for the prevention or treatment of melasma or postinflammatory hyperpigmentation has been established.
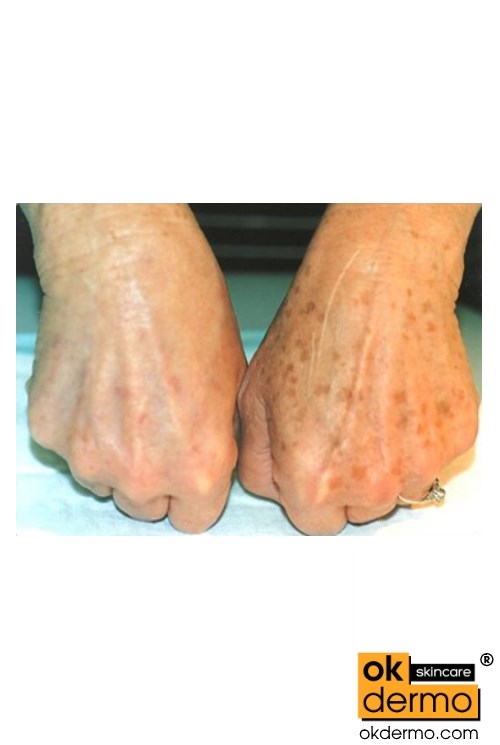
Solar lentigines – are sharply circumscribed, uniformly pigmented macules that are located predominantly on the sun-exposed areas of the skin, such as the dorsum of the hands, the shoulders, and the scalp. Lentigines are a result of hyperplasia of keratinocytes and melanocytes, with increased accumulation of melanin in the keratinocytes. They are induced by ultraviolet light exposure.
Unlike freckles, solar lentigines persist indefinitely. Nearly 90% of Caucasians over the age of 60 years have these lesions. Due to the increased prevalence of lentigines in the elderly, these lesions are sometimes referred to as “lentigo senilis”. However, younger individuals who tend to burn after ultraviolet exposure can also develop lentigines after acute or prolonged ultraviolet light exposure. Clinically, solar lentigines may be oval, round, or irregular in shape and can vary from a few millimeters to a few centimeters in diameter. Most lesions have a uniform light brown color; however, there are instances when they vary from dark brown to black.
One variant of solar lentigo, “ink-spot” lentigo, has a jet-black color. Actinic purpura or other signs of solar damage can frequently be found in the skin surrounding solar lentigines. Solar lentigines are benign lesions that can evolve to a pigmented seborrheic keratosis. Histologically, it is characterized by club-shaped rete ridges with small nub-like extensions. In addition, there is an increased number of melanocytes and increased pigmentation in the basal keratinocytes. Although most solar lentigines are easily recognized on clinical examination, some lesions pose diagnostic challenges because their clinical appearance resembles that of melanoma. Dermoscopy can be helpful in correctly differentiating a solar lentigo from melanoma. The key dermoscopic features of solar lentigines are as follows:
Liver spots / Age spots – Liver spots (also known as age spot, solar lentigo, “lentigo senilis”, “old age spot”, “senile freckle”) are blemishes on the skin associated with aging and exposure to ultraviolet radiation from the sun. They range in color from light brown to red or black and are located in areas most often exposed to the sun, particularly the hands, face, shoulders, arms and forehead, and the scalp if bald.
The spots derive their name from the fact that they were once incorrectly believed to be caused by liver problems, but they are physiologically unrelated to the liver, save for a similar color. From the age of 40 onward, the skin is less able to regenerate from sun exposure, and liver spots are very common in this age group, particularly in those who spend time in the sun.
In the overwhelming majority of cases, liver spots pose no threat and require no treatment, though they occasionally have been known to obscure the detection of skin cancer. However, despite being a benign condition, liver spots are sometimes considered unsightly and some people choose to have them removed. This can be done by electrosurgery, laser treatment, cryotherapy, or the use of depigmentation agents, such as hydroquinone, tretinoin, topical cysteamine, azelaic acid or alpha hydroxy acids.
Differently from the melanotic nevi and the verrucous nevi on the skin, age spots change with time in color and in shape. Misrepair-accumulation aging theory proposes a hypothesis on the development of age spots. Firstly, the development of a flat spot is a result of the accumulation of aged basal cells. When the skin is aged, some aged cells that contain lipofuscin bodies cannot be removed. An aged cell will affect the functionality of the local tissue and promote the aging of its neighbor cells. By a feedback loop, more and more neighbor cells become aged and lipofuscin-containing. They aggregate and form a spot with an irregular shape. Secondly, protruding of a flat spot is a result of the death of aged cells in the spot and release of lipofuscin bodies. Isolation of the un-digestible lipofuscin bodies in a fibrotic capsule is essential for maintaining the structural integrity of the tissue. Successive encapsulation of dead cells and lipofuscin bodies results in the growth of a spot in three dimensions. The dense lipofuscin bodies in the capsule make a protruding spot soft and dark in color.
HOW IS MELALONG MEQUINOL 2% + TRETINOIN 0.01% CREAM USED
Melalong cream should only be applied topically once per day at bedtime unless otherwise directed by a dermatologist or skin care specialist. Wash the cream off the skin thoroughly in the morning before heading outdoors. Contact dermatologist for the correct dosage and length of treatment as it will depend on user condition and their response to the therapy. It is recommended to apply sunscreen if you intend to head outdoors after washing off the Melalong medicated cream.
MELALONG MEQUINOL 2% + TRETINOIN 0.01% CREAM SIDE EFFECTS
Melalong (Generic Solage) cream with low concentration Mequinol 2% and Tretinoin 0.01% is generally very well tolerated but may cause minor side effects such as dry skin, erythematous lesions, white patches at the application site, increased sensitivity to the sun, contact a dermatologist immediately should side effects persist or worsen. Seek medical advice if you suffer an allergic reaction. Symptoms usually associated with such a reaction include difficulty breathing or swallowing, chest tightness, swelling, skin rashes, and hives.
Melalong Mequinol 2% and Tretinoin 0.01% cream is not always suitable for all. Always consult your dermatologist prior to using this medicated cream if you are pregnant, breastfeeding, trying to conceive, using any other medication, using any herbal products or supplements, or if you have any allergies or other health problems. The correct dosage commonly depends on the patient and the condition being treated. Do not adjust your dosage without the approval of your dermatologist. This product is only for use as prescribed and instructed by professionals.
HOW TO GET RID OF BROWN HORMONAL SPOTS
Melasma is a type of skin hyperpigmentation typically characterized by brown or gray discoloration of the face. It is commonly found in women with darker skin types, though men and women of all races may be affected. While the exact cause of melasma discoloration is unknown, the condition is commonly associated with hormone fluctuations triggered by pregnancy, oral contraceptives and hormone replacement therapy.
There is no cure for melasma. After giving birth or stopping hormone therapy, the condition may fade on its own. When dealing with persistent brown hormonal spots, recommended following a regimen of sun protection, exfoliation, and bleaching to reverse the normal skin color and gradient.
First of all skin protection. Select a broad-spectrum sunscreen with an SPF of at least 30. When exposed to sunlight, hyperpigmented skin gets darker than surrounding areas. This makes sun protection crucial to the reduction of melasma. Wear sunscreen throughout the day. Apply sunscreen 30 minutes before sun exposure. Reapply every few hours. Wear a wide-brimmed hat to further protect your face from harmful UV rays.
Treat your skin. Wash and dry your face. Apply a lotion or cream containing glycolic acid all over your face. Glycolic acid is a mild chemical exfoliant that treats melasma by removing superficial pigmented skin cells and easing the penetration of bleaching agents. Wait 20 minutes, then apply a small amount of Melalong a 2 percent Mequinol and 0.01% Tretinoin cream to the melasma-affected skin. Hydroquinone/Mequinol 2% is a chemical bleaching agent; over time, it fades hyperpigmentation by stopping melanin production on treated skin areas. Do not recommend to use hydroquinone longer than 4-5 months in a row. Wash hands thoroughly, then apply sunscreen.
Even weak Glycolic acid 6% cream formulations can cause irritation; to avoid damaging skin, start with a lower concentration and if necessary, increase the strength over time. Treat dark hormonal spots every day. Some hydroquinone 2 percent products recommend twice daily applications, but better to use once per day before bedtime, read the included instructions to determine proper dosing and use. It can take three to six months for melasma to improve. Glycolic acid and hydroquinone 2% can increase sun sensitivity. Wear sunscreen at all times and limit sun exposure. Long-term hydroquinone 2% use may cause ochronosis, a darkening of the treated area of skin. Hydroquinone 2% is not suitable for pregnant or breastfeeding individuals as well.